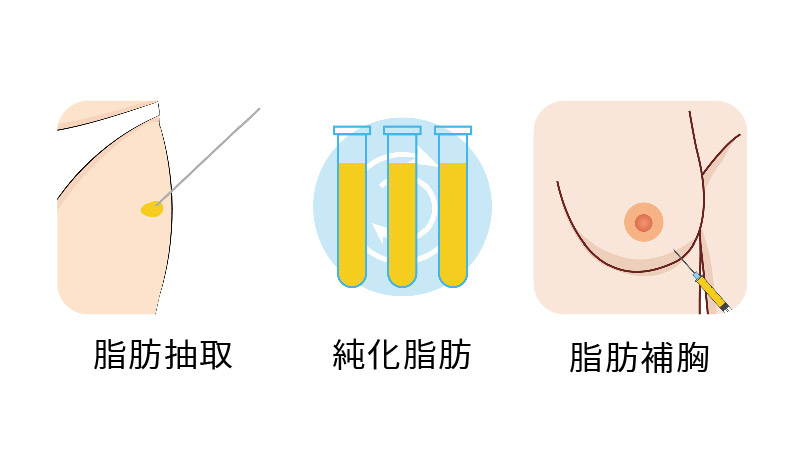
自體脂肪隆乳手術是一種利用自身脂肪進行隆乳和豐胸的手術。手術過程中,醫師使用抽脂儀器從腹部、臀部、手臂、大腿等脂肪較多的部位抽取多餘的脂肪。這些脂肪經過特殊的離心純化處理,以獲得純淨的奈米脂肪,再注入到胸部進行多層次填充,從而達到隆乳和豐胸的效果。
女性的胸部是其重要的性徵之一,不僅關係到身體美感,還與女性的自我形象和社會角色密切相關。然而,一些因素如天生乳房發育不良、妊娠和哺乳後乳房萎縮變形、以及天生不對稱等問題,常常導致女性對其自身形象感到不滿。
在此情況下,自體脂肪移植隆乳手術被視為一種安全有效的選擇。來自日本和韓國的學者進行研究後發現,將抽取的脂肪分為兩份,然後對其中一份進行純化處理,可以提高移植後脂肪的存活率,進一步增加手術的成功率。


誰適合做自體脂肪隆乳?
- 乳房發育不佳過於平坦
- 乳房大小或位置胸型不對稱
- 懷孕產後輕度下垂鬆弛
- 過度減肥造成胸部鬆弛
- 胸部大小不滿意
- 義乳取出重建、淡化義乳明顯邊緣
- 期望完全真實觸感、避免義乳異物感
- 隱藏隆乳手術後的疤痕
自體脂肪隆乳手術原理流程
- 局部麻醉或全身麻醉:您會接受舒眠麻醉,以使其在手術期間感到無痛或輕微不適。
- 提取脂肪組織:醫生會從腹部、手臂或大腿等脂肪較豐富的部位提取脂肪組織。這個過程可能需要幾個小時,具體時間取決於提取的脂肪量和使用的技術。
- 純化脂肪組織:提取脂肪組織後,會將其離心處理和血水過濾,以去除多餘的油脂和雜質組織。
- 注射脂肪組織:邱正宏醫師會使用沙拉式打法(Solid Injection Method),用細小的針頭在乳房/臉部/臀部等不夠豐滿的的位置注射脂肪,以達到預期的效果。
- 術後觀察恢復:手術完成後,您需要在診所內觀察一段時間,以確保手術順利完成並檢查有無異常。通常情況下,可以在幾天之內恢復正常的日常活動,並在數週後回到正常的運動活動中。
自體脂肪隆乳使用自身的脂肪,因此沒有過敏或排斥的風險。手術後,不需要按摩也不能按摩,且胸型看起來自然,不會像假體一樣有邊界球感。隆乳手術後的舒適度和自然度都比較好。
自體脂肪隆乳手術的成功關鍵主要取決於脂肪存活率,包括先天體質、醫師施打注射脂肪技術和術後照護等,這些因素會影響脂肪在隆乳區域的存活率。在景升診所,平均存活率約為70%,隆乳手術三個月後,留下的脂肪可半永久存在,但是隨著年齡和體型的自然變化,可能會有一定程度的變化。如果希望升級多個罩杯大小,建議需要進行兩次以上的手術。
自體脂肪隆乳缺點優點?
| 優點 | 缺點 |
|---|---|
| 安全性高: 使用自身的脂肪細胞進行注射,不需要外部物質,因此排斥反應和感染的風險較低。 | 體重變化會影響效果: 由於自體脂肪移植豐胸是利用抽取的自身脂肪進行隆乳,因此若體重有大幅度變化,可能會影響效果,甚至需要進行補注射。 |
| 自然度高: 可以達到比較自然的效果,因為注射的是自己的脂肪細胞,與周圍組織相容性更好,可以更好地融入原有的乳房組織。 | 隆乳效果較其他方式較低: 相較於使用乳房植入物進行隆乳,自體脂肪移植豐胸的隆乳效果較低,因為注射的脂肪量有限,且部分脂肪細胞在手術後可能會吸收,影響隆乳效果。 |
| 同步身材雕塑: 需要抽取身體脂肪,可以同時改善身體其他部位的脂肪分布,例如腰部、臀部、腹部、大腿、手臂等等。 | 需要脂肪充足: 需要足夠的脂肪儲備才能進行,如果脂肪不足,可能無法達到理想效果。 |
| 手術後恢復快: 不需要植入假體,手術傷口小,恢復期較短,也不需要按摩,通常可以在幾天到一週內回復正常活動。 | 可能需要多次手術: 如果需要進行大量脂肪注射,可能需要進行多次手術,每次注射的脂肪量也有限制,需要等待一段時間才能進行下一次。 |
自體脂肪移植豐胸手術是一種安全有效的隆乳方式,具有自然度高、手術恢復快、兼顧身體其他部位等優點。但也存在著隆乳效果較低、需要脂肪充足、體重變化會影響效果等缺點。如果您考慮進行隆乳手術,可以與專業醫生進行詳細諮詢和評估,以確定是否適合進行自體脂肪移植豐胸手術。

自體脂肪隆乳術前術後注意事項
| 術前注意事項 | 術後注意事項 |
|---|---|
| 告知用藥狀況與過往乳房手術、乳癌家族病史紀錄。 | 胸部避免激烈碰撞與晃動,術後運動視恢復狀況與醫師確認 |
| 術前一週停用阿斯匹靈、吃維他命E、進補、喝四物飲 | 術後三個月是黃金期,這段時間不能減肥減脂,影響隆乳效果 |
| 蟹足腫或肥厚疤痕體質者、有服用抗凝血劑成分藥物者應告知醫師。 | 多補充蛋白質等營養,像是魚湯、牛肉湯、豆漿牛奶都非常適合 |
| 術前一個月避免抽菸、喝酒。 | 避免按摩胸部、避免胸部重壓、避免側睡/臥睡、喝蜈蚣草等中藥。 |
| 手術前最好先乳癌篩檢及乳房攝影,術後定期乳房檢查。 可協助早期發現乳房異常病變,提高治療效果,減少風險。 | 術後定期回診追蹤。兩個月內避免高溫場所(例如泡熱水澡或三溫暖),以免傷口未癒合造成感染。 |
自體脂肪隆乳手術是利用自己身體的脂肪進行隆乳,相較於使用人造物質,具有較低的手術風險和更自然的外觀效果。然而,手術前後的注意事項仍然是至關重要的。
首先,在手術前,會進行詳細的身體檢查,以確定是否適合進行手術。此外,手術前還需要進行血液檢查和心電圖檢查等必要檢查,以確保身體健康狀態符合手術條件。
手術後,需要嚴格遵循醫師的建議,避免過度活動和避免負重,以促進傷口的癒合。此外,還需要按時服用藥物和照顧傷口,避免感染和其他併發症。
除此之外,定期追蹤檢查也是必不可少的。遵循醫師的建議,定期進行乳房檢查和超音波檢查,以確保自己的身體狀況良好,並及早發現任何潛在的問題。這樣可以最大程度地減少手術後的風險,並確保手術的成功。
2024 自體脂肪隆乳PTT Q&A 常見問答解析
自體脂肪隆乳需要多久回診一次?
自體脂肪隆乳手術後需要定期回診以確認手術部位的恢復情況和隆乳後的效果。回診的時間間隔可能會因人而有些許差異,但通常是以下情況:第一次回診:通常是在手術後2週,回診拆線以及確認手術後的恢復狀況。第二次回診:通常是在手術後3個月,這時候乳房和抽脂處通常已經穩定,醫師會做乳房超音波檢查確認脂肪存活的情況和乳房的健康程度,並和客人探討後續是否需要進一步的處理。之後的回診通常每隔6個月至1年進行一次。請注意,以上回診時間僅供參考,實際時間會因個人情況和手術方式而有所不同。在手術後,請務必遵從醫生的指導,按時回診以確保自體脂肪隆乳術後的健康和效果。
自體脂肪隆乳術後需要按摩嗎?
自體脂肪隆乳後,不需要按摩。跟假體隆乳不一樣,假體隆乳後需要按摩,是為了減少假體外的莢膜反應,自體脂肪隆乳沒有這種問題,所以不需要按摩。另外,自體脂肪隆乳後,按摩反而會將脂肪擠壓破壞,導致脂肪的死亡,最終降低脂肪的存活率,所以,過度擠、壓、捏、撞,都應該避免。這種照顧原則,至少要維持三個月,一直到移植的脂肪穩定後才可以。所以,做完自體脂肪隆乳手術後,至少三個月內都不應該在胸部上按摩、或擠壓。至於抽脂區的照顧,如果過了兩三個星期,不會疼痛以後,就可以適度的按摩,讓腫脹儘速消除,針對腫脹不均的地方,也可以儘速平復。
自體脂肪隆乳多少錢?
抽脂和隆乳的費用因地區、診所、手術範圍和手術方法等因素而異。台灣的抽脂和隆乳手術費用也因此會有所差異。一般來說,抽脂手術的費用大約在新台幣6萬元至15萬元之間,隆乳手術的費用則約為新台幣15萬元至30萬元之間。但這僅供參考,具體的費用需根據實際情況進行評估和確定。另外,手術費用可能不包括術前檢查、手術後的藥物治療、恢復期間的醫療照顧等附加費用,需要考慮到整個手術流程的全面費用。如果您有興趣進行抽脂或隆乳手術,建議您與當地的診所或醫生聯繫,進行詳細的諮詢和評估。
自體脂肪隆乳可以一次抽出多少脂肪呢?
手術需要抽取足夠的脂肪來注射到乳房中,以達到期望的效果。通常,一次需抽取至少1200毫升的脂肪。但是實際抽取的脂肪量取決於個人情況(例如脂肪分佈和身體質量指數等),以及醫生的建議和手術計劃。有些可能需要進行多次手術,以獲得期望的效果。在手術前,醫生會進行詳細的身體檢查和評估,以確定最適合您的手術計劃。
自體脂肪隆乳後遺症?
所有手術都有可能產生後遺症,自體脂肪移植豐胸也不例外。但是,相較於其他乳房隆乳手術方法,自體脂肪隆乳的風險較低,因為使用的是自身的脂肪細胞,減少了排斥反應和感染的風險。以下是可能出現的一些後遺症:1. 脂肪細胞存活率低:部分注射的脂肪細胞可能無法正常存活,導致乳房大小不平衡或不夠飽滿。2. 感染:手術後可能會出現感染,因此需要遵循醫生的建議,進行正確的護理和清潔。3. 脂肪囊塊:在部分案例中,可能會出現脂肪囊塊,這些囊塊可能會影響手術效果,需要進行二次注射或手術來解決。4. 不均勻:注射脂肪細胞可能導致乳房不均勻,需要進行微調和修復。5. 瘢痕(蟹足腫)形成:手術後可能會出現瘢痕形成,需要進行治療。
自體脂肪隆乳手術可以增加幾個罩杯?
自體脂肪移植隆乳手術的術後效果因多種因素而異,包括個人體質、手術技術、脂肪吸收率等。平均來說可以增加1-2個罩杯的大小,但不能保證所有人都能達到相同的效果。景升診所以其豐富的臨床經驗和純熟的技術而聞名,在自體脂肪隆乳手術方面已累積數萬例成功案例,其中部分不僅增加2個罩杯的大小,甚至有的案例可以增加2至4個罩杯的大小。

自體脂肪隆乳和假體隆乳有什麼差異?
| 手術方式 | 自體脂肪隆乳手術 | 果凍矽膠假體隆乳手術 |
|---|---|---|
| 隆乳方式 | 利用自身脂肪注射進行隆乳 | 植入人工乳房植入物進行隆乳 |
| 外觀和感覺 | 比較自然,看起來和觸感和自身乳房類似 | 感覺比較硬,有時候比較明顯 |
| 手術傷口 | 較小,通常只有抽取脂肪的傷口 | 比較大,植入人工乳房需要開刀 |
| 操作部位 | 脂肪提取部位和隆乳部位 | 隆乳部位 |
| 術後按摩 | 不需按摩 | 需按摩 |
| 優點 | 外觀觸感自然美觀 | 尺寸多樣化可自行選擇 |
| 缺點 | 單次補脂程度有限 | 後遺症較多 |
| 恢復時間 | 恢復較快,通常幾天到一週左右 | 需要較長的恢復時間,通常需要幾週到幾個月 |
| 隆乳效果 | 隆乳效果較低,一次注射的脂肪量有限,且部分脂肪細胞在手術後可能會吸收,影響隆乳效果 | 隆乳效果較高,可以根據您的需求進行精確大小的隆乳 |
提到「隆乳」,大多聯想到在體內裝果凍矽膠的義乳行隆乳手術,而「自體脂肪移植豐胸」採用身體特定部位多餘脂肪,取出純化後轉移至胸部,達到隆乳與調整胸型的效果。
使用自己的脂肪來填充,乳房觸感的自然度是其他假體無法比擬的,不敢裝義乳在體內、希望低調升級、想要脂肪再利用的女性,自體脂肪移植豐胸手術是非常好的選擇。
自體脂肪隆乳後悔ptt? 看看成功案例現身說法!

珠珠身高168公分、體重44公斤,BMI 15.5 非常纖細,自體脂肪隆乳給她真實又豐滿的乳房。
莎莎身高160公分,體重40公斤,骨架纖細,自體脂肪隆乳給她真實又豐滿的乳房。

看更多自體脂肪移植豐胸手術案例:


